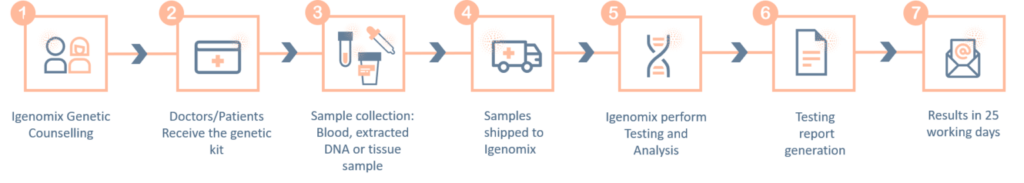
Systemic Lupus Erythematosus Precision Panel
Systemic Lupus Erythematosus is a chronic multisystemic autoimmune disease of unknown cause. The most prominent feature of this disease is the onset of immunologic abnormalities, especially the production of antinuclear antibodies.