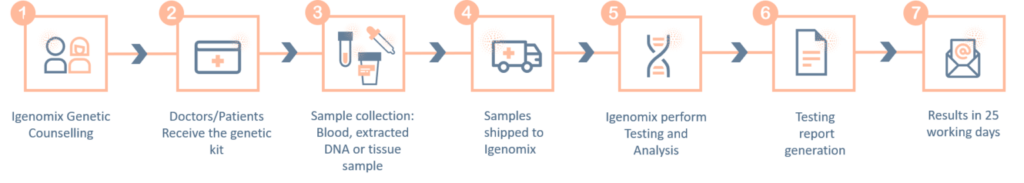
Xeroderma Pigmentosum Precision Panel
Xeroderma Pigmentosum (XP) is a rare autosomal recessive disorder characterized by photosensitivity with easy skin burning following minimal sun exposure, pigmentary changes, premature skin aging and predisposition to malignant tumor development.