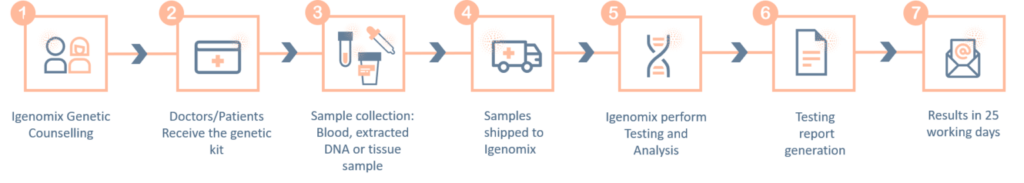
Oculocutaneous Albinism Precision Panel
Albinism is a group of inherited abnormalities of melanin synthesis and are characterized by a decrease or absence of melanin pigment. There are several types of albinism, one of them being oculocutaneous albinism (OCA).